Four Reasons Your Knee Pain isn’t Going Away
Approximately 25% of adults suffer from chronic knee pain and for many, they don’t have a clear reason or diagnosis as to why. They’ve been told to accept that their knee pain is due to arthritis, age, or wear and tear. So why then, are some people able to get rid of their pain with proper knee pain treatment while others continue to suffer? It starts with the correct diagnosis. And for many chronic knee pain sufferers, this is the problem.
Here are four reasons why your knee pain might not be going away:
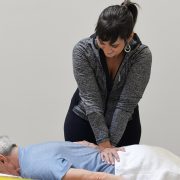
1. Mobility Before Stability
I’m a firm believer in this concept.
Our joints function better when they have full and free mobility. With knees in particular, everyone tends to focus on how well a knee is bending, but a lot of people miss when a knee isn’t fully straightening. Most knees have a certain amount of what we call hyperextension.
For example, your knee might look and feel straight, but if it’s naturally capable of “over-straightening”, and you don’t restore that completely, your knee will have problems.
I see it all the time, especially in folks who’ve had previous knee surgeries. If their full knee motion wasn’t restored properly during rehab, or perhaps they didn’t have any rehab at all (common practice now after most arthroscopic knee surgeries), knee pain will persist, and won’t go away no matter how much you strengthen it.
This isn’t something that can be seen on an Xray or MRI. Only a trained expert who knows how to look for this will be able to detect it, teach you how to restore it, and finally help you get rid of your chronic knee pain.
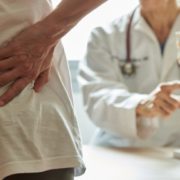
2. It’s Really a Back Problem
When the source of your pain is truly coming from your knee, it tends to be pretty specific and very localized to the knee joint itself. But if your pain tends to move around your knee, or perhaps travel up and down your leg, there’s a good chance your knee pain is coming from your back.
A recent study found that 40% of all extremity pain (including knees) comes from a source in your spine – even when you don’t have any back pain.
How does this happen? Typically it’s due to an irritated nerve that sends pain primarily to your knee and nowhere else. If you’ve been treating your knee for months and it’s either not going away or perhaps getting worse, consider that your knee problem is not a knee problem. Get your spine checked by a proper movement/mechanical therapist who can screen for this and figure it out.
3. Poor Core Strength
Your abdominals, low back muscles, hips, and glutes all make up what we call your “powerhouse” or core.
We all know that a strong core is important to help prevent back pain. But, it’s equally important for healthy knees. If your core is weak, or doesn’t activate properly, it will have an impact on how fluid your joints will move during activities.
If you aren’t stabilizing yourself well with a strong core, your knees might try to help out by adding stability. Knees aren’t really meant to do this – they are meant to be mobile. But when your body lacks stability, your joints stiffen up in response, which can cause knee pain over time or aggravate arthritis that’s already there.
If your knees chronically ache – especially during activities – this could be why. You can treat your knees all you want, but if you don’t also address the deficits in your core, your knees will continue to hurt.
4. Stiff Ankles
When your ankles are stiff it will have an impact on your knees.
Do one or both of your ankles lack mobility during certain activities? Especially running, hiking, and squatting? Your knees may strain themselves trying to help out and compensate.
Over time, this pattern will lead to knee pain. Do you notice a lot of stiffness in the front of your ankles? Or pain/fatigue in the front of your lower legs after repetitive walking or running? This could be a sign that the real problem is coming from stiffness in your ankles.
Stop working on your knees and start mobilizing your ankles instead. Your knees should start to feel better in no time. Knee pain can be tricky to figure out – especially if it’s chronic. Arthritis, age, and wear and tear aren’t common reasons for chronic knee pain. But they are definitely reasons that mislead people into thinking they’ve just got “bad knees”.
At least 70% of the time, knee pain can be resolved naturally and with movement – but you must make sure you’ve got the correct diagnosis nailed down first.
Want some help getting rid of YOUR knee pain?
Talk to one of my specialists for free by CLICKING HERE.
Dr. Carrie Jose, Physical Therapist and Pilates expert, owns CJ Physical Therapy & Pilates in Portsmouth and writes for Seacoast Media Group. To request a copy of her Knee Pain Free Report CLICK HERE or to get in touch, email her at [email protected].