Why More People are Paying out of Pocket for Healthcare…even during an economic downturn
More People are Paying out of Pocket for Healthcare…even during a recession
If you’ve ever had an injury or dealt with chronic pain, you’ve probably followed a pretty traditional course of action to address it that might have looked like this:
- You went to your primary care doctor and they sent you to the lab for x rays, prescribed medication, or both.
- You may have gotten a referral to a specialist or even a surgeon.
- You went to that appointment and were either told that you needed surgery or that you needed to modify your physical activity and avoid certain activities in order to not exacerbate the problem.
Basically, you were thrust into the assembly line that has become “modern healthcare”.
But did you know that you could bypass all of this hassle – and get faster results – by going directly to a physical therapist?
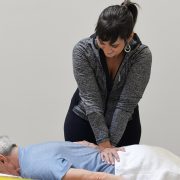
Physical therapists are trained to diagnose your problem and provide a fully customized treatment option. One that doesn’t involve prescription medications or procedures.
In almost all states (including NH) you don’t even need a prescription to see a physical therapist.
The problem is that for many people, traditional physical therapy has not produced the results they are looking for.
Physical therapy DOES work. But what often doesn’t work is the model of care.
There have been many limitations insurance companies have placed on reimbursement over the years. Most traditional physical therapy clinics (those that take insurance) have been forced to see more patients. Just so they can pay the bills and keep the lights on!
Additionally, insurance companies and healthcare have essentially taken over your care.
They decide who you can see, what type of treatment you will get, and how many visits you are allowed to have.
These decisions are being made by someone who’s never even spoken to you, met you, or actually looked at you.
Because of this, “physical therapy” has gotten a bad reputation and a lot of people find that it’s a waste of time, or that it consists of just a bunch of exercises.
It’s not the physical therapist’s fault, it’s the insurance company’s fault.
The good news is that you’ve got options and alternatives when it comes to taking care of your back or knee pain.
You don’t want to be prescribed medication and you don’t want to deal with procedures like injections or surgery. Or you don’t want to go to traditional physical therapy and feel like you’re wasting your time. The answer is to go outside of your insurance and pay out of pocket.
This is known as going “out of network”.
More people are doing it because they are fed up with the traditional models. Models of healthcare and physical therapy that don’t give them the results they are looking for.
But isn’t that expensive? Not at all, and it really depends on what you value.
For me, and for most of the folks that we work with, it’s far more costly to live with chronic back pain. You have to miss out on activities you love, and end up with a surgery you never even wanted.
It’s also far more costly to spend years going to weekly chiropractic and massage therapy appointments. Just so that you can function and manage your pain.
When it comes to musculoskeletal problems, you NEED a physical therapist in your corner and as part of your healthcare team.
But it can’t be the traditional kind where all you get is cookie cutter treatment plans. Physical therapists who don’t contract with insurance companies are able to spend more time with you. Allowing them to create a truly customized plan of care.
We focus on getting to know you and your body. Not what paperwork needs to be filled out for your next healthcare insurance authorization.
Our clients like this model because they get long-term success instead of short-term pain relief. Our therapists like this model. They are free to use their brains and actually do what they were trained to do.
Everyone should have their own, personal physical therapist to call and come see anytime you need. Just like you would a chiropractor, dentist, doctor, or massage therapist.
The only way to do this, is to go outside your insurance. If you are curious about whether or not this model of physical therapy is right for you just give us a call!
It’s not for everyone, but more and more people are finding that it is.
Most of the folks we meet and work with say: “I wish I had found you first”.
If this is something you are interested in – or are seeking more information on – CLICK HERE to speak to one of my specialists.
They will give you all the information you need to make the BEST decision for YOUR health. Whether that’s working with us or not!
Dr. Carrie Jose, Physical Therapist and Pilates expert, owns CJ Physical Therapy & Pilates in Portsmouth and writes for Seacoast Media Group. To get in touch, or request a free copy of one of her guides to back, neck, knee, or shoulder pain, email her at [email protected].