Running Over 50: Top 3 Injuries and What you can Do
If you love to run, then you’re probably no stranger to running injuries.
But if you love to run and you’re over 50, not only are you more likely to suffer a running-related injury compared to runners half your age, but you’ll tend to suffer from different categories of injuries as well. In older runners, we tend to see more soft-tissue related injuries versus problems with joints and stress fractures. Part of this is due to the fact that older runners may have been running longer. This predisposes them to more long-term wear and tear that is typically associated with soft tissue injuries like tendinopathy and plantar fasciitis. Older runners also are more likely to have altered their running mechanics over time, another factor that leads to injury. Either way, the good news is that once you know what to look for, you can take proactive measures to prevent these common running injuries as well as treat them naturally.
Here are the top 3 running injuries I see in people over 50 and what you can do:
1. Plantar Fasciitis
Plantar fasciitis is a condition characterized by a sharp, stabbing pain in your heel or bottom of your foot. It often worsens with the first steps in the morning or after long periods of rest. This discomfort comes from inflammation in your plantar fascia, a thick band of tissue running across the bottom of your foot from your heel to your toes. Factors such as overuse, improper footwear, high arches, flat feet, and tight calf muscles can all contribute to the development of plantar fasciitis, whether you’re a runner or not.
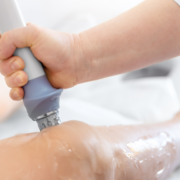
Prevention measures for plantar fasciitis include incorporating regular stretching and self-massaging of your plantar fascia and calf muscles before and after running. Balance exercises that focus on strengthening the intrinsic muscles of your foot, along with maintaining a healthy weight can also help – as it will allow you to better control and manage the load that gets transmitted through your plantar fascia. But what if you’re already suffering from pain due to plantar fasciitis? Don’t just resort to rest and ice, which has been known to impede healing. Plantar fasciitis requires prescriptive loading of your muscles in order to remodel the damaged tissue. This, along with non-invasive treatments such as Shockwave Therapy designed to enhance blood flow to the tissue, can aid in accelerating your healing.
2. Runner’s Knee (Patellofemoral Pain Syndrome)
Runner’s knee is a term used to describe a variety of conditions that cause pain around the kneecap (patella) – and is often synonymous with patellar tendonitis. You’ll notice your runner’s knee most during activities that require knee bending, walking downhill, or descending stairs. Overuse of your quadriceps muscles, poor tracking of your patella, and any other muscle or joint imbalance that results in increased load to the front of your knee can all result in runner’s knee.
Regular and balanced strength training of the muscles around your knee – particularly of the quadriceps, hamstrings, and hip muscles – is a key prevention strategy. Making sure you have good ankle and foot mobility is also important. Because if your foot doesn’t move well when you run, unwanted forces move up the chain into your knee, eventually leading to runner’s knee. If you’re already suffering from runner’s knee, then you’ll want to first mitigate your pain. Similar to plantar fasciitis – rest and ice won’t do much for you. Getting blood flow to the area – followed by carefully prescribed exercises designed to restore your mechanics and properly load your patella tendon – is what’s going to heal the irritated tissue in and around your knee and make it stronger.
3. Achilles Tendinitis
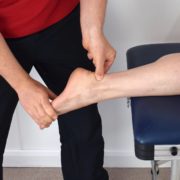
Achilles tendinitis presents as pain and swelling in the back of your heel or lower calf. Right where your Achilles tendon connects your calf muscles to your heel bone. Your Achilles pain will typically be most prominent during or after running. It may be accompanied by stiffness when flexing your foot. While the causes of Achilles tendinitis are very similar to that of plantar fasciitis, we see this occur most often with sudden increases in intensity or duration of training. Particularly, this happens when your body is not adequately prepared.
A gradual increase in training load, regular calf strengthening and stretching exercises, and proper warm-up and cool-down regimens can go a long way in preventing Achilles tendinitis. Be cautious of your footwear as well. Minimalist running shoes have become extremely popular. But, if you move into them too quickly, your Achilles tendon could become irritated due to the sudden change in load and force. If you’re already suffering from Achilles tendinitis, the treatment is quite similar to that of plantar fasciitis. The exception is that when it comes to tissue loading, you’ll want to focus more on your lower calf and Achilles tendon, versus the plantar fascia.
With all of these conditions, keeping yourself healthy and in good shape is crucial for prevention.
Enlisting the help of a running coach is also a good idea. They can address any potential issues with your running mechanics that may have occurred over the years. If you’re picking up running for the first time, or returning to it later in life, take it slow and easy. Consider talking to a movement expert who can detect and analyze any imbalances in your body. They can ensure that you’re moving and exercising correctly. Imbalances will cause you to compensate. This is not something that will be immediately obvious to you – until it’s too late.