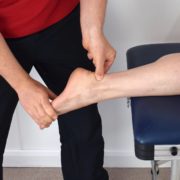
Tendonitis versus Tendinosis: The Big Difference and Why it Matters
Tendonitis is a term you’re likely familiar with. You’ve probably even suffered from it at some point in your life. It’s an acute, short-term, inflammatory condition typically caused by repetitive overuse of your tendon. Tendinosis, on the other hand, is a chronic, degenerative condition of your tendon. It involves deterioration of collagen, a structural protein in your tendon. While the two conditions sound very similar, and are often used interchangeably, they couldn’t be more different. And the treatment for each condition should be different too.
Tendons are tight but flexible bands of fibrous tissue that connect your muscle to bone.
Without tendons, your muscles would be useless. Tendons are extremely organized, and the fibers are designed in a way to withstand and transmit high forces of tension so your muscle can function properly.
With tendonitis, your tendon becomes inflamed and irritated, typically due to repetitive overuse.
Tendonitis causes pain when you try to move. The most common areas for tendonitis to occur are your elbows, rotator cuff (shoulder), patella (knee), and Achilles tendon (ankle). Tendonitis is an acute condition, and the best treatment is to rest, apply ice, and sometimes take anti-inflammatories to control pain. From there, you want to figure out what caused the tendonitis to occur in the first place and address that. Typically, it’s due to some sort of mismatch between muscle strength and the activity you need to perform, leading your body to compensate and put unwanted stress on your tendon. Once you figure out and correct this pattern, it’s very easy to get rid of your tendonitis!
When you don’t manage tendonitis properly, and it goes on longer than a few months, it can result in tendinosis.
Tendinosis is a very different condition where the fibers in your tendon actually start to break down. An important thing to note is that tendinosis no longer involves inflammation of your tendon. So using ice every day, resting it, and taking anti-inflammatories will not help you. I can’t tell you how many times I’ve spoken to people still doing this 6-8 months after an unresolved tendonitis issue. Second, since tendinosis involves disorganization and degeneration of the fibers that make up your tendon, you have to “re-organize” those fibers in order to resolve tendinosis and get your tendon functioning properly again.
Passive treatments like ice, rest, and medicine will not help tendinosis.
They might help to relieve any pain you’re having from overdoing it or undertreating it — but the tendinosis will continue to progress. Unresolved tendinosis leads to progressive weakening of your tendon over time, making it easily susceptible to full blown tears. This is how so many folks tear their Achilles tendon or rotator cuff, for example, “out of nowhere.” Once I speak with them, they often report that over the years they had recurring bouts of tendonitis in that area. In other words, their tendonitis wasn’t managed properly and it led to chronic tendinosis, making them an easy target for a torn tendon.
So how do you treat tendinosis and prevent more serious problems from happening down the line?
You have to re-organize those fibers so your tendon can work properly again! Sounds easy, right? Well technically it is, but the biggest problem is that this process takes time, up to 9 months in many cases. And most patients I come across simply don’t have the patience for this… or they simply aren’t told. The other issue is that if you’re expecting an insurance company to cover your treatment, they typically don’t want you in physical therapy for more than 6-12 weeks at a time. This is not long enough to properly treat tendinosis.
The only way to re-organize those tendons is to put stress on them.
You have to put just the right amount of stress to cause a little bit of pain, but not so much that your tendon gets inflamed again. This is literally the one time where “no pain no gain” is actually true. A properly trained physical therapist who is well-versed in tendinosis will know how to do this. You basically have to retrain the fibers to withstand force again – and this process takes time. The good news, however, is that if you rehab your tendinosis properly, you can get back to all the activities you love as if nothing ever happened!
If you’re confused after reading this, don’t worry – so is half the medical community. The take home points to remember are that tendonitis involves pain and inflammation, there is no damage to your tendon, and it only lasts about 4-6 weeks. Treatment for this should involve passive modalities like ice and rest, and the focus should be on what caused your tendon to get irritated in the first place.
But if problems in your tendon have gone on longer than 3 months, you must suspect tendinosis, which no longer involves inflammation but instead, a breakdown of your tendon. Passive treatments will NOT work and could actually prolong your problem – so stop icing and resting. Getting rid of tendinosis requires carefully prescribed loading strategies (aka strengthening) that will properly re-organize your tendon so that it can be strong again! This is extremely challenging to do on your own, so it’s a good idea to talk to an expert about this. You can even schedule a FREE Discovery Session with one of our experts today!