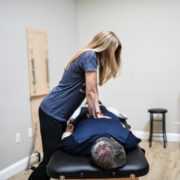
Battling Sciatica? Here’s what to Avoid and what you should do Instead
Did you know that nearly four out of five people will suffer from a debilitating back pain episode at some point in their lives and that it can result in sciatica?
“Sciatica” is a term used to describe searing pain, burning, or numbness that runs from your back and down your leg, often below your knee and into your foot. It occurs because something in your lower back is irritating the nerve that sends signals to your leg. It can be caused by anything that puts pressure on and/or irritates your sciatic nerve – such as herniated or bulging discs.
What a lot of people don’t know is that you can have sciatic symptoms without actually having any back pain. Sciatic symptoms can occur just in one place in your leg – like your knee and/or foot – or run down the whole leg as described above. Regardless of how your sciatica is behaving – there are some general “best practices” that almost all versions of sciatica will respond to.
Here’s what you should avoid when you’re battling sciatica – as well as what to do instead:
What to Avoid:
1. Soft beds and couches
While it may feel better in the moment – lying in soft beds or couches will ultimately aggravate your sciatica. When you lie in soft beds or couches – it forces you into a slouched posture – which puts unwanted pressure on your already irritated nerves. What’s tricky is that you often won’t notice the aggravation while you’re in the slouched position. It won’t be until later, perhaps when you get up to walk or move around, that you’ll feel worse. Because of this, people mistakenly attribute the aggravation of their sciatica to the activity they just did instead of the prolonged, slouched position they were assuming perhaps just minutes or hours before.
2. Child’s pose and stretching forward.
Just because a stretch feels good, doesn’t mean it is good – another big misconception when it comes to sciatica. Since sciatica is often caused by a bulging or herniated disc that is putting pressure on your nerve – you want to avoid anything that is going to increase that pressure. When you stretch forward – like in child’s pose – you’re opening up the space in between your vertebrae (intervertebral space). In between each vertebrae lies your discs. Although it feels good “in the moment” when you’re stretching forward – and may even temporarily relieve your sciatica – this relief won’t last. By opening up your intervertebral space – you’re making it easier for your discs to protrude out and irritate your nerves – unknowingly prolonging or worsening your sciatica.
3. Letting your MRI dictate treatment.
As already mentioned, sciatica often involves bulging discs – and an MRI will typically confirm this. But here’s what you might not know… Research has shown us that lots of folks (more than 60%) have bulging discs showing up on their MRI’s, but they don’t all have back pain or sciatic symptoms. What that means is that while sciatica is often caused by a bulging disc, a bulging disc doesn’t always guarantee you’ll have sciatica. Why is this important? Because when you allow your MRI findings to dictate your treatment plan, you’re more likely to undergo a procedure or surgery that might not be necessary. Removing the bulging disc material or fusing your spine together might take the pressure off the nerve temporarily, but if the underlying issue is a movement or mechanical problem, and it’s not addressed, it’s only a matter of time before your problem comes back and/or shows up in a different area of your spine.
What to Do:
1. Go for Walks.
Walking is one of the best things you can do for back pain – even though it may seem counterintuitive to do so when you’ve got pain running down your leg. Walking is an upright activity that is generally good for sciatica versus the slouched, curved posture you have when sitting. When you walk, pay close attention to what happens in your leg. Do your symptoms worsen or start to get better? If they worsen, certainly stop and seek professional guidance. But if your leg starts feeling better – then the walking is likely good for your sciatica.
2. Pay attention to your Posture.
This may seem trivial – but maintaining good posture is critical when you’re suffering from sciatica. When your sciatic nerve is irritated, it becomes highly sensitive to postural changes in your lower back (especially slouched postures). Whether you’re sitting or standing – you want to maintain the natural S-curve of your spine as best as you can. I recommend to my clients they use a lumbar roll whenever they are sitting to make maintaining this posture easier. Correcting your posture alone is often not enough to get rid of your sciatica, but it can keep you from getting worse, and prevent it from coming back if you’ve successfully eliminated your sciatic symptoms.
3. Talk to a Mechanical Pain Specialist.
Did you know that 70-80% of all musculoskeletal pain is mechanical in nature? Both back pain and sciatica can fall into this “mechanical pain” category – which is caused by slowly developing movement problems or habits that eventually result in stiffness and mobility restrictions in your spine. These restrictions can lead to irritated structures, such as nerves. So if your sciatica is due to a mechanical problem – it’s not going to permanently improve with pills, procedures or surgery. You’ll need to find a mechanical pain specialist who can help correct and restore your movement patterns for a long-term solution you can maintain on your own.
Dr. Carrie Jose, Physical Therapist and Pilates expert, owns CJ Physical Therapy & Pilates in Portsmouth and writes for Seacoast Media Group. To request a free copy of her guide to back pain CLICK HERE or to get in touch, email her at [email protected].