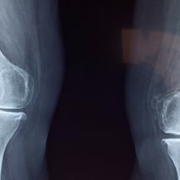
Torn Meniscus? Is Surgery Worth it?
It’s estimated that approximately 750,000 arthroscopic knee surgeries are performed every year – the majority of them being due to a torn meniscus.
But at a cost of about $4 billion per year – is this surgery even worth it?
Let’s investigate…
Arthroscopic knee surgery is a minimally invasive procedure that’s commonly done to help “clean out” your knee joint if you’ve got degenerative arthritis, or to clip out pieces of a torn meniscus that might be irritating your knee. The biggest set of pro’s for this procedure is that it’s quick, recovery is fairly minimal, and you will typically experience an immediate relief of pain.
Sounds worth it – right?
Not so fast. There are many cons to this procedure as well, many of which are not realized until it’s too late. So it’s worth a second opinion and considering all of your options before you jump in.
First, as with any surgical procedure, even if it’s minimally invasive, there are risks. Complications include nerve damage, excessive bleeding, infection, reactions to anesthesia, persistent stiffness and swelling, or blood clots. While these risks tend to be rare, they don’t outweigh the other long-term considerations you should be aware of.
Looking to avoid a knee replacement in your future?
Then you’ll definitely want to think twice about getting arthroscopic meniscus surgery. Research tells us that people who undergo arthroscopic knee surgery are likely to have knee arthritis that advances more rapidly – resulting in a total knee replacement that quite possibly could have been avoided. This is because you’re removing vital cushioning and shock absorbing mechanisms (the meniscus) from your knee joint. Plus, a meta-analysis published in Oct 2020 in the Knee Surgery, Sports, Traumatology, Arthroscopy journal revealed a 36% failure rate by year two – and a 13% failure rate by year five for meniscus repairs – resulting in more surgery and eventual knee replacement.
And then there’s the elephant in the room…
It’s more common than you think for knee pain to be coming from somewhere other than your knee, even when your MRI shows a meniscus tear. Knee pain can be caused by problems in your ankle, hip, or back. One study showed that 40% of the time – knee pain comes from a source in your spine – even when you don’t have any back pain. MRI’s add even more confusion to this because degenerative changes, which are normal as we age and very commonly lead to a torn meniscus, make surgeons think your meniscus is the cause of your knee pain when it might not be. The only way to truly determine the cause of your knee pain (in the absence of trauma) is through a proper mechanical exam that involves repeated movement testing to reveal the actual pain generator.
The truth is – 70-80% of all knee problems can be resolved naturally and without surgery.
An early research study from 2002 by JB Mosely and colleagues, and published in the New England Journal of Medicine, revealed that placebo surgery for advanced knee arthritis was just as effective as actual arthroscopic surgery. Since then, numerous studies have proven similar results. This means that even if you have a torn meniscus or degenerative arthritis in your knee – you can still get better naturally and with conservative treatment.
So why then – despite all this research – are surgeons still performing arthroscopic knee surgery to repair a torn meniscus?
In some cases it’s just what the surgeon knows, and they haven’t kept up with the research. Other times, it’s due to poor conservative management of knee pain. If you’ve gotten physical therapy and it wasn’t effective, people are led to believe that the physical therapy “didn’t work”. But more often than not, you didn’t get physical therapy from a specialist – someone who understands how to diagnose knee pain properly and get you the customized approach that is required to avoid surgery.
If you’re young and involved in high-level sports, meniscus surgery is likely worth it for you.
But for most people, especially those over the age of 40, there’s a 70-80% chance you can get full relief of your knee pain, and full restoration of knee function without any type of surgery or procedure. This is not a popular opinion by the way, so be careful who you speak to for a second opinion. But for me, both the research as well as my 22 years of clinical experience tell me that most people (especially those over age 40) can resolve their knee pain naturally and with better long-term results if they avoid arthroscopic knee surgery – even when there’s a meniscus tear.